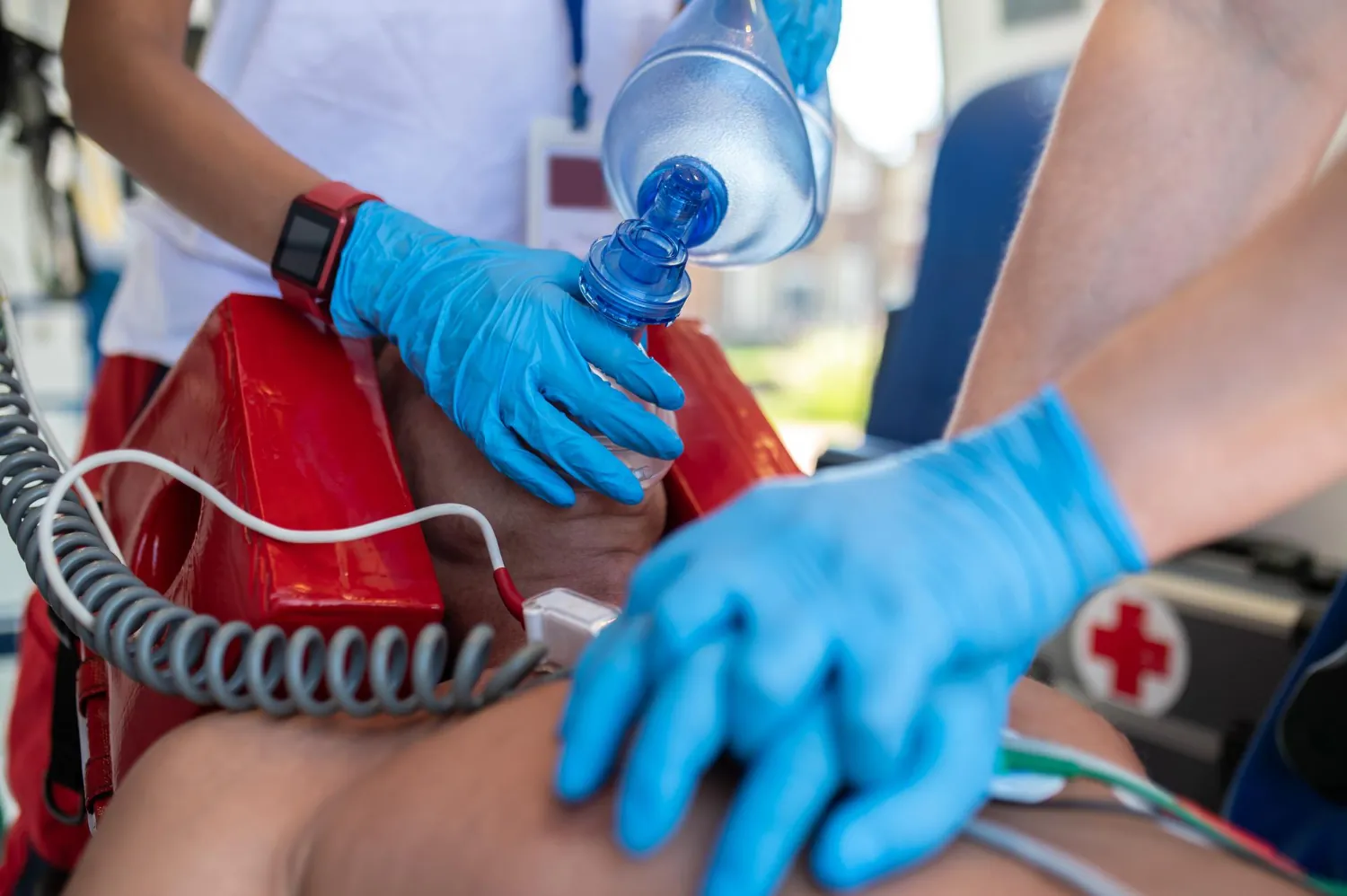
10 Signs of Paramedic PTSD

According to paramedic PTSD statistics, first responders have a much higher rate of traumatic stress than the general population.
We all know that burnout can happen, especially in our high-stress field, when we see traumatic events on a regular basis. If you or a colleague is experiencing signs of PTSD in EMS, it's time to seek assistance. Here's how to identify some of the common signs of paramedic PTSD.
What to Do if You Suspect PTSD
Right up front, it's important that if you suspect PTSD or high-stress levels, you get help immediately. Stress reactions can escalate quickly, leading to substance abuse, exhaustion, and suicidal ideation. It's not something to ignore, hoping it will just go away.
The other thing to know about PTSD is that it's common and not something that can be controlled or "powered through." It's also not just something that happens to civilians who experience a natural disaster or traumatic experience. Combat veterans, firefighters, police officers, and emergency professionals-some of the toughest people in the world-all have a greater risk of PTSD. There's no shame in having a stress response to extreme stimuli, and the development of PTSD is not controlled by the person experiencing the trauma, nor is it their fault.
Years ago, PTSD had a stigma of sorts, but in today's world, that stigma has long since passed. As a protector and defender of fellow human beings, you want to prioritize your physical and mental health. It's important to address the symptoms of PTSD right away. The sooner it's addressed, the more effective the treatment will be.
Several organizations are working to end any remaining stigma behind mental health conditions and support first responders and emergency personnel experiencing stress and chronic PTSD symptoms. There are plenty of effective treatment options that can help those at the greatest risk for PTSD and related mental health issues.
The Code Green Campaign gets its name from the common language of emergency response, "code X," and green, the color of mental health awareness. They work to help emergency responders find support when they're experiencing stress on the job.
Safe Call Now is another service for all public safety employees. They offer confidential support and emergency mental health services referrals for all public safety workers throughout the United States. Call the number and get assistance if you feel a colleague needs help or support. The UK has similar organizations, including PTSDUK.
Finally, the United States recently launched the 988 Lifeline program, which provides suicide prevention services confidentially, 24 hours a day, to people of all ages. If you're experiencing these feelings, it's crucial to reach out. There are people who will listen and understand.
10 Signs of PTSD in EMS
Maybe you aren't sure if what you're experiencing is a stress reaction. For many people, especially those who have worked in a high-stress job for a while, it can be hard to recognize the signs of too much stress. Paramedics and first responders enter the field because they love what they do (and don't mind the adrenaline rush), so it can be tough to admit, even to yourself, that you may need to take a break or address your stress.
Supervisors and colleagues should also familiarize themselves with the signs of PTSD in EMS. Sometimes, others can pick up on the cues before we realize them ourselves or have a diagnosis of PTSD. If you notice a coworker showing signs of paramedic PTSD, it's crucial to say something. Offer support, listen, and communicate. In emergency response, we're all stronger when we can communicate openly with our team.
The following symptoms of post-traumatic stress disorder might be pronounced or subtle. They may come on slowly or present themselves suddenly all at once. Here's what to watch out for:
1. Nervousness, anxiety and agitation
If you aren't usually anxious but suddenly feel nervous, antsy, or easily irritated, it can be a sign of too much stress. Staying calm under pressure is the nature of emergency response, but we all freeze up or feel fear well up in our chests every so often. Anxiety disorders can develop at any time. Feeling nervous or stressed is natural and human, but when it becomes frequent, it could be a sign of something more.
Stay aware of your feelings during your work. Check in with yourself occasionally, and if you need to take a break or step away to regroup, share that with your team. At the same time, if a team member suddenly seems anxious and agitated, encourage them to take a breather.
2. Lapses in concentration, memory, or clear-thinking
Everyone forgets now and then, but if you have difficulty remembering important steps-especially on the job, it could be a sign that you're experiencing higher stress levels. If your mind suddenly goes blank, rely on your muscle memory and focus on making the next step. Breathe through the moment.
Again, everyone has a moment when they forget or "space out" on something, but concentration and clear thinking are vital when lives are on the line. If you feel foggy (or your team member is struggling), take a break. If it happens multiple times or seems to last a long time, it's time to address the stress. Stress can mar a person's ability to make decisions and think clearly.
3. Moodiness and emotional breaks
Our emotions are 100% valid as human beings. As first responders, we can see some tough scenes on the job. It's particularly tough to see children and those who are vulnerable, injured, or sick on a regular basis. Feeling emotional isn't a bad thing.
On the job, however, we often have to push those emotions down to stay present in the moment. After we leave the scene, we might find that those feelings come out as moodiness, anger, sadness, or tearfulness. We might lash out at family members or isolate ourselves. Another sign of PTSD is experiencing emotions that feel too strong or disproportionate to the moment.
4. Depression and suicidal thoughts
Feeling like you can't control your emotions or that you're having a trauma response can be upsetting. It can lead to feelings of sadness, hopelessness, and despair. Emotional reactions are bound to occur. We can also see situations on the job that can be very upsetting and sad, and EMS workers care deeply for those they serve.
Depression can take over, causing us to feel demotivated and even paralyzed from moving forward. If you suddenly feel like your days are devoid of joy, you can't get out of bed, or you have suicidal thoughts, it's critical that you get help.
5. Physical discomfort like headaches, chest tightness, shakiness
Sometimes, we might not feel the stress in our emotions, but it can manifest in our bodies and harm our physical health. Warning signs of stress include headaches, chest tightness, muscle aches, jaw pain, shoulder tension, dizziness, shakiness, and digestive issues. We would identify many of these symptoms in our patients as signs of panic or anxiety, but sometimes, it's tougher to notice in ourselves.
Of course, if you experience any sudden or new physical issues, it's crucial to go to the doctor to get it checked out. If you can't nail it down to any specific physical illness or problem, it's time to examine the mind-body connection.
6. Panic attacks and waves of paranoia
Like some of the physical discomfort symptoms of stress, panic attacks can cause physical and emotional symptoms. They can come on suddenly and intensely or present a low level of paranoia and anxiety that you can't shake. You might just feel like "something is wrong."
Emergency responders know the signs of panic attacks because we see them often in our patients. But we might not always pick up on these feelings in ourselves or our colleagues. If you're feeling stressed, take some time to check yourself. If you suspect a panic reaction, talk to someone to get to the bottom of it.
7. Sleep disturbances
Sleep issues are another major sign of too much stress. While none of the symptoms outlined here indicate PTSD on their own, when several of them are combined, it can mean that you may have PTSD or chronic PTSD. Most people have nightmares or moments when they can't get their sleep under control. But when it happens continuously, it can wear you down and exacerbate stress. Sleep disturbances are among the risk factors for many mental health problems, including PTSD.
Good sleep is vital for optimal health and performance. If our sleep is disrupted for multiple nights, we can find ourselves making mistakes, experiencing brain fog, and having a short temper. For first responders, sleep is mandatory. If you feel like stress is bleeding into your slumber, it can wear you down fast.
8. Hypervigilance and "magical thinking"
Hypervigilance is the feeling that you need to check everything over and over. You need to consider every possibility. You need to be diligent, or you're responsible for anything that goes wrong. Similarly, magical thinking can include thoughts of, "If I do X, then Y won't happen." Noticing negative changes in your thought patterns on a daily basis can interrupt day-to-day life and exacerbate stress.
Both of these modes of thinking often come about when we feel a lack of control over our circumstances or a situation. Our brains tell us we need to do better next time to prevent it. We need to check and double-check or perform rituals (like touching the outside of the bus before you board). While a little superstition is pretty common, these feelings can interfere with clear thoughts and make it hard to recognize reality.
9. Ruminating thoughts and flashbacks
Maybe you find yourself playing traumatic memories like a car accident again and again. Perhaps you think, "I just can't let it go," and you fixate on the moment, playing it repeatedly. These repeated thoughts are called ruminations. When we ruminate, we focus on thoughts we can't move past.
Flashbacks and ruminations can feel very prevalent and intense. They might occur constantly or only when we're trying to relax. We may have sudden flashes seemingly out of nowhere or find that something reminds us of a traumatic moment and starts the loop of our internal video.
10. Desire to "numb" the response
Substance use and alcohol abuse are common ways to deal with stress. For emergency responders, we might find that we want a drink to unwind. One drink becomes two, and then four. Chronic stress might lead to drug use. While we might turn to substances to numb our feelings, they can worsen our stress.
The other major concern with substance abuse in EMS is that we have constant access to an array of controlled substances that we can also turn to. This is how diversion happens and why it's important to recognize problems before the temptation becomes too great.
Helping Stress in Emergency Response
PTSD isn't something to feel any shame over. It's something that we should all familiarize ourselves with and be aware of in case we start to feel some of the symptoms of PTSD. Asking for help will get us back on track and back on the job before we burn out or get in over our heads.
One way that supervisors and leaders in EMS can help is by fostering communication channels. Offer support services without shame. Listen to your team; don't push them to ignore or "play through the pain."
Emergency response is stressful, but it can become a little easier with the right tools. LogRx is one tool that can help you and your team members track controlled substances used on the job. Rather than relying on paper logs to keep track of inventory and report scheduled drugs, LogRx works right from your team's handheld devices. They can report on the go in real-time.
LogRx makes it easy for administration, too. From our admin portal, you'll have access to an array of reports and helpful tracking tools. Check inventory levels, prevent diversion, and make reporting simple. It's almost like having an extra member on your team!
Contact us today if you'd like to explore ways to make your reporting and tracking simple. We work with emergency responders, law enforcement, veterinarians, wildlife professionals, air ambulances, and more. Anyone who handles controlled substances on the job can benefit from the ease of LogRx tracking!
Categories
Recent Posts
- LogRx and Knox: How LogRx Integrates with EMS Medication Lockboxes
- Connecting Community and EMS: 7 EMS Community Outreach Ideas
- Projecting Professionalism: Why EMS Uniforms Matter
- EMT Off-Duty Response: What You Should Carry Everywhere
- Basic EMT Trauma Assessment Scenarios: Gearing Up for Certification















.webp?t=1779916840388)